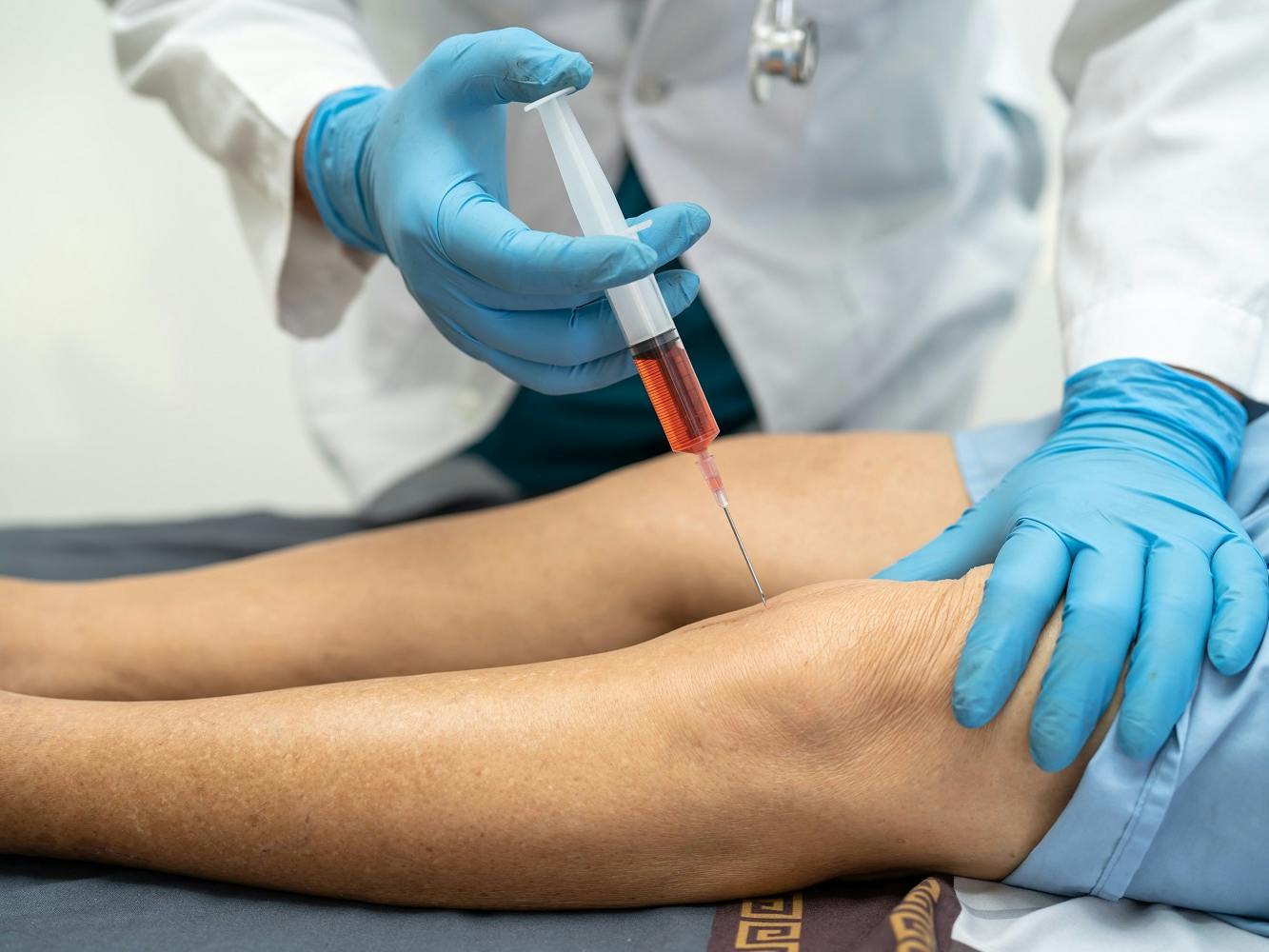
Knee injections can relieve joint pain and stiffness, even if only temporarily. Medicare may cover knee injections, if you qualify.
Throughout your lifetime, even healthy joints experience a great deal of wear and tear. This is especially true for your knees, which help support your entire bodyweight. Throw in a chronic condition like arthritis, a sprain here, a strain there, and it's no wonder most adults experience knee pain at some point.
Even with the reduction in non-emergency surgeries due to COVID, there were over 2.2 million knee and hip replacements in 2021, according to the American Academy of Orthopaedic Surgeons. But before your healthcare provider recommends something as invasive as a total knee replacement, they'll likely begin with more conservative treatments, like supports and, in the case of chronic pain, knee injections.
We'll start by looking at some of the common causes of chronic knee pain, so you can better understand your Medicare coverage.
What causes chronic knee pain?
The most common causes of knee pain are related to aging, injury (such as sprained or strained knee ligaments and/or muscles, torn cartilage, or tendonitis), or repeated stress on the knee.
Osteoarthritis is the most common type of arthritis that affects the knee and is very common in adults as they age. Osteoarthritis is a degenerative process where the cartilage in the joint gradually wears away. It is typically caused by excess stress on the joint, such as repeated injury or being overweight.
Rheumatoid arthritis can also affect the knees, causing them to become inflamed and destroying knee cartilage. However, this often impacts a person at an earlier age than osteoarthritis.
Typically, diagnosing a knee problem includes a medical exam and diagnostic procedure such as X-ray, MRI, CT scan, or arthroscopy.
Both noninvasive and surgical treatments are options for treating knee pain, depending on the type and severity of your condition.
When to see a doctor for knee pain
Some symptoms and signs of arthritis or related joint conditions include:
- Pain, swelling, tenderness, or stiffness
- Joints that are red or warm to the touch
- Difficulty moving a joint
You should schedule an appointment with your primary care provider (PCP) if your joint symptoms last three or more days or you have several episodes of joint symptoms within a month. Your PCP will determine whether you need to see a specialist, such as a rheumatologist or orthopedist, and give you a referral if necessary.
What are knee injections?
As the name implies, knee injections are shots that help relieve pain and inflammation in the knee joint. These treatments are generally considered safer, less expensive, and lower risk than alternative treatments (like surgery) and they require little or no recovery time.
Knee injections typically provide fast relief, but the relief is also temporary. However, this allows you to participate in regular day-to-day activities.
Different types of knee injections
The most common types of knee injections include corticosteroids and hyaluronic acid injections (HA), also known as viscosupplementation.
Corticosteroids
Corticosteroid injections can help reduce pain and inflammation when injected into the knee or other joints. You may start to experience relief within 24 hours. However, relief typically only lasts for two to three months, and a patient may only receive a limited number of these injections per year.
Hyaluronic acid injections (HA) or viscosupplementation
More simply known as knee gel injections, these shots can reduce pain and inflammation by mimicking the effects of natural joint fluid. It helps lubricate the worn-down joint, facilitate better movement, reduce pain, and slow the progression of the osteoarthritis. They are best for patients with diabetes, because unlike corticosteroid shots, they do not raise blood sugar levels.
This treatment typically takes about two weeks to feel the full effects, but relief can last six months to one year. One common HA injection is Euflexxa, and Gel-One is another.
Are knee injections covered by Medicare?
As long as the injections are considered medically necessary, Medicare will cover some types of knee injections once every six months. Because these injections are typically administered by a physician in a medical office or clinic, they are covered by Part B (medical insurance).
Note that x-rays are required before Medicare approval. These would also be covered by Medicare Part B if considered medically necessary. For injections to be covered, you must show evidence of knee osteoarthritis with X-rays, and you may be limited to a certain number of injections per year.
You would pay 20% of the Medicare-approved amount for these injections after meeting the Part B deductible ($226 in 2023).
Does Medicare Advantage cover knee injections?
Medicare Advantage plans are required by law to cover everything Original Medicare does (Parts A and B). So, if the treatment is covered by Medicare, it will be covered by your Advantage plan.
Part C plans aren't limited to those benefits, though. And most of them, 99%, provide additional benefits in the form of things like routine dental and vision, fitness benefits, and prescription drug coverage. Since private insurance companies sell Medicare Advantage plans, costs and benefits differ. Check your plan's Evidence of Coverage or call your plan provider for details.
What does Medigap cover?
Medicare Supplement Insurance, more commonly known as Medigap, does not provide additional benefits. Instead, a Medigap plan will pay your out-of-pocket costs when you have Original Medicare. How much the plan pays depends on which plan you choose. There are 10 standardized Medicare Supplement plans. Eight cover the Medicare Part B coinsurance at 100%. Two, Plan K and Plan L, cover it at 50% and 75%, respectively.
It's important to note that you cannot use a Medicare Supplement plan to pay for items not covered by Original Medicare. For more information, please see our Ultimate Guide to Medigap.
Alternative treatments for knee pain
Corticosteroid injections are often the first step in treating knee pain. However, in addition to knee injections, there are some other ways to treat knee pain.
One of the most noninvasive ways to help relieve current and prevent future knee pain is by walking. Regular, brisk walking for at least 30 minutes can not only help with knee pain, but also improve your mood; reduce stress; support a healthy weight; improve your heart health, blood pressure, and cholesterol; boost muscle and bone strength; and more.
Typically, arthritis affects the inner portion of the knee, making it wobble toward the inner part of the knee when walking. This makes it so that the knee joint doesn’t wear down evenly. An unloader knee brace is designed to limit the side-to-side movement of the knee and can help force the knee to bend away from the painful joint area. This may be considered durable medical equipment (DME) and would be covered by Part B.
Nerve therapy can be an option for patients who have nerves of the knee pinched by the worn-down knee. This outpatient procedure may be covered by Part B.
Platelet-rich plasma (PRP) shots use a patient’s own plasma to promote healing of soft tissue and reduce inflammation. This treatment is most frequently used to treat osteoarthritis because it has a low risk and limited side effects, but these shots are typically not covered by Medicare.
And, while it’s a major procedure that may require weeks or months of preparation before and recovery after, knee replacement surgery may be an option. This procedure and related services may be covered by both Medicare Part A and Part B.
How to prevent knee pain
The best way to prevent knee pain, especially as you age, is to stay active, such as by:
- Walking
- Swimming
- Low-impact exercise
- Weight training (after consulting an expert)
Maintaining your weight is important because extra weight can increase your chances of developing osteoarthritis. Additionally, be sure to wear sensible shoes with a good fit to help you maintain proper leg alignment and balance. Try not to decrease your activity level, which can lead to weakness, and don’t suddenly change the intensity of your exercise. Instead, gradually build it up.
We have a great article on how to start lifting weights if you're over 60 here.
Additional resources
- ClearMatch Medicare: Find a Medicare Plan
- American Academy of Orthopaedic Surgeons: American Joint Replacement Registry 2021 Annual Report



