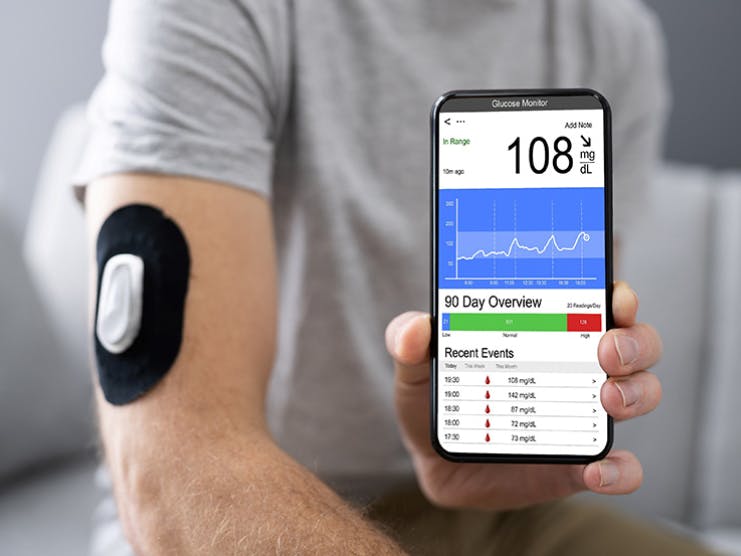
A continuous glucose monitoring system like Dexcom G6 can help control your diabetes – but will Medicare help pay for it?
Diabetes care can be tricky depending on the type you have and how well you manage it. The good news is that glucose monitoring technology, such as continuous glucose monitoring systems (CGM), makes managing your diabetes and glucose levels easier.
Instead of pricking your finger several times a day to check your blood glucose levels, using new technology can provide real-time data 24 hours a day. This helps you continuously monitor your levels without taking up time, requiring you to remember to take measurements, or missing measurements because you’re sleeping or busy.
While these systems can be beneficial, it’s important to know if they are covered by insurance. Read on to learn if Dexcom G6, a CGM system, is covered by Medicare, how it works, and what other diabetes supplies are also covered.
What are continuous glucose monitors?
Continuous glucose monitors and related supplies for making diabetes treatment decisions are covered by Medicare Part B, as long as the device is considered durable medical equipment.
These blood glucose monitors automatically track blood glucose levels, or blood sugar. A person can see their glucose level anytime and review how it changes over a few hours or days to find trends, which allows them to make better decisions about balancing food, exercise, and medication.
A CGM works by placing a tiny sensor under your skin (typically the belly or arm). This sensor monitors your interstitial glucose level, which is glucose found in the fluid between your body’s cells. The sensor does this every few minutes, and the information is sent wirelessly to a monitor. These monitors can be part of an insulin pump or could be a separate device.
The best thing about CGMs is that they are always working, and some even have special features to help you better manage your diabetes, such as an alarm when your glucose levels go too high or too low or tracking your meals and exercise in a CGM device.
The primary benefits are better managing your glucose, having fewer low blood glucose emergencies, and needing fewer finger sticks.
Is Dexcom G6 covered by Medicare?
The Dexcom G6 Continuous Glucose Monitoring System is covered by Medicare, as long as you meet coverage criteria. In fact, Dexcom will ship the Dexcom G6 to Medicare patients with traditional fee-for-service coverage, or you can get one at your local Walgreens or through a durable medical equipment (DME) supplier.
Dexcom G6 Medicare coverage criteria
For a Medicare beneficiary to have coverage for a Dexcom G6 CGM System, they must:
- Have either type 1 or type 2 diabetes
- Be insulin-treated with three or more daily administrations of insulin, or a continuous subcutaneous insulin infusion (CSII) pump
- Have an insulin treatment regimen that requires frequent adjustments based on BGM or CGM testing results
- Have had an in-person visit with their provider within six months prior to ordering the CGM in order to evaluate their diabetes control and determine coverage criteria is met
To remain covered, beneficiaries must have an in-person visit with their provider every six months following the initial prescription of the CGM to assess adherence to the regimen and diabetes treatment plan.
Medicare also requires you have a receiver that’s compatible with a Dexcom G6 and you use that receiver with your supplies.
Dexcom G6 supplies used only with a mobile device or other smart device are not covered.
Medicare diabetes coverage
CGM supplies and accessories are covered by Medicare when the beneficiary uses a receiver classified as DME to display glucose data. Medicare Part B covers several other types of diabetic equipment and supplies including:
- Blood sugar self-testing equipment and supplies, including blood sugar monitors, blood sugar test strips, lancet devices and lancets, and glucose control solutions
- Insulin pumps
- Therapeutic shoes or inserts
To receive coverage, you must have a prescription by your doctor.
There are other services covered as well, such as diabetes screenings, the Medicare Diabetes Prevention Program, Diabetes Self-Management Training, and Medical Nutrition Therapy (MNT) services.
Foot exams and treatment, hemoglobin A1C tests, and glaucoma tests are also covered if you meet certain eligibility criteria.
Additional Resources
Introduction to Dexcom CGM
External Website Link
Continuous Glucose Monitors
External Website Link
Medicare Guidelines for Insulin Pump Approval
Internal Website Link
What Medical Equipment Does Medicare Pay For?
Internal Website Link



