Medicaid income limits vary not only by state, but also whether you’re an “individual” or a parent.
While some Medicaid provisions are required by federal law, many aspects are decided by each individual state. Additional benefits, qualifications, and income limits are all set at the state level. Income limits are based on the federal poverty level, with each state basing those limits as a percentage of the federal poverty level.
What is Medicaid Redetermination?
Before the COVID-19 pandemic, most states did a yearly income and resource evaluation to ensure people receiving Medicaid benefits were still eligible. This is called Medicaid Redetermination.
Part of the U.S. government’s COVID response was declaring a Public Health Emergency. Next, as part of the Families First Coronavirus Response Act, the federal government offered increased funding for state Medicaid programs, so long as the state paused redetermination. This ensured millions of people wouldn’t lose their health insurance (in this case, Medicaid) during a global pandemic.
With the end of the Public Health Emergency, this protection is now over. Medicaid Redetermination began again on April 1, 2023.
Will I lose Medicaid coverage?
Completing the Medicaid Redetermination process takes time, so you may still have coverage even after April 1, 2023. In addition, if you are determined to be ineligible, you will not immediately lose coverage. State Medicaid programs have to send you a notice and provide 30 days for you to respond. If you do not respond, the state follows up with a 10-day notice.
If you currently receive Medicaid benefits and are worried about losing coverage, the best thing to do is be proactive. Make sure your state Medicaid office has your current information and be sure to provide any information it may request as soon as possible.
Complete the redetermination form on your Medicaid program’s website, and check in periodically to see if your status has been updated. You generally have to provide your current address, household size, income, and documentation to back up this information.
If you are 65 or older, you should enroll in Medicare. Typically, people lose Medicaid coverage based on their age (i.e., because they age into Medicare eligibility), income, or simply not providing enough information.
There are still options for you if you lose your coverage after Medicaid Redetermination.
If you are under 65 and lose coverage, the Centers for Medicare and Medicaid Services (CMS) announced a Special Enrollment Period (SEP). From March 31, 2023 through July 31, 2023, you can enroll in a new Marketplace health plan.
If you are over 65, losing Medicaid coverage qualifies you for a Medicare SEP that lets you sign up outside of standard enrollment periods. The SEP lasts for three months from either the date you lost coverage or the date you were notified, whichever is later. During this time, you can sign up for Original Medicare (Part A and Part B).
Once you have Parts A and B, you may then join a Medicare Part D prescription drug plan. You may also enroll in a Medicare Advantage or Medicare Supplement (Medigap) plan.
You can learn more about Medicare Redetermination and what that means for you here.
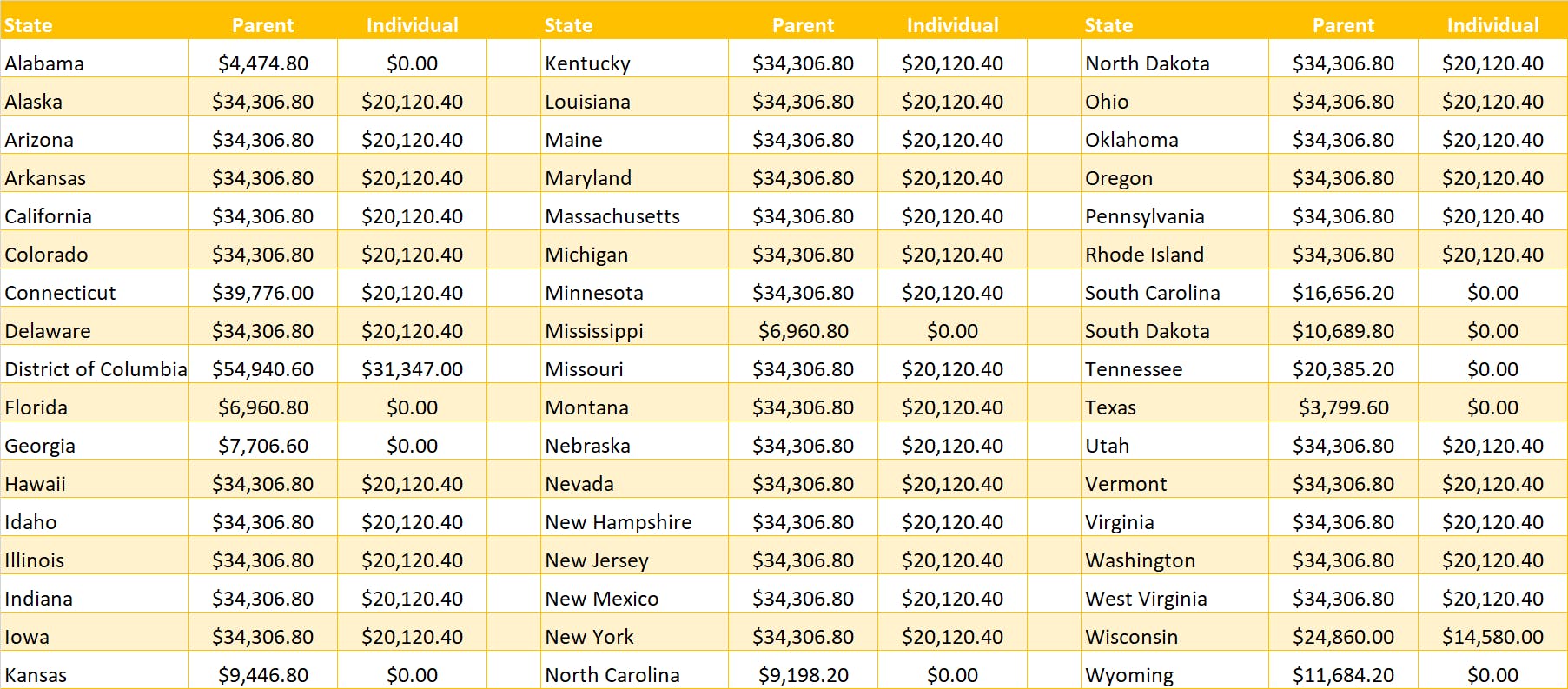
Medicaid income limits
As stated above, income limits for Medicaid are decided state by state and are based on the federal poverty level.
The federal poverty level for parents of dependent children is $24,860 in 2023.
The federal poverty level for other adults (individuals) is $14,580 in 2023. Below are the Medicaid income limits for both categories for each state.
Additional resources
Find a Medicare Plan
Internal Website Link



