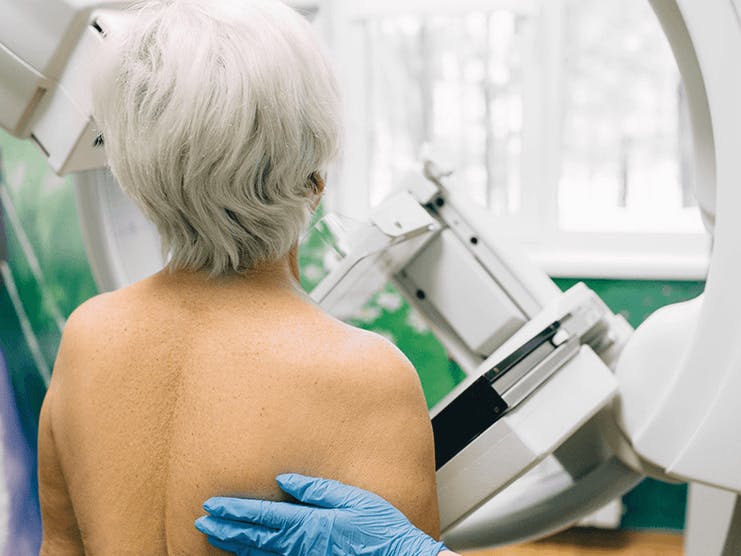
Regular mammograms can help detect breast cancer three years earlier than you would feel a lump.
One in eight U.S. women will develop breast cancer over the course of her life.
In 2021, more than 300,000 new cases of breast cancer were diagnosed in women in the U.S., and as of January 2021, more than 3.8 million women had a history of breast cancer.
Even though it's now the most commonly diagnosed cancer among American women, some forms of breast cancer can be prevented, treated, and irradicated successfully. The first step in protecting yourself and lowering your risk of developing breast cancer is by getting regular screening mammograms.
How often does Medicare cover mammograms?
Medicare Part B covers:
- One baseline mammogram for women ages 35-39
- Screening mammograms once every 12 months if you're a woman aged 40 or older
You pay $0 for a screening mammogram if your provider accepts assignment. This applies for both 2D and 3D mammograms, as well as a digital mammogram.
Diagnostic mammograms are covered more frequently than once per year if it's medically necessary, though you'd pay 20% of the Medicare-approved amount and the Part B deductible applies.
It's recommended that women between the ages of 50-74 have a screening mammogram every year, though your doctor may recommend additional screenings. Medicare mammogram coverage doesn't stop at a particular year, so women in their 80s, 90s, or even 100s can still get a screening or diagnostic mammogram and it will be covered.
What is a mammogram?
Breast cancer develops when cells in the breast grow out of control. There are several different types of breast cancer depending on which cells in the breast turn into cancer. Then, breast cancer can spread outside the breast through blood vessels and lymph vessels, which can make it more difficult to treat.
When you get a mammogram, you'll stand at a special x-ray machine. A technologist will place your breast on a plastic plate, and a second plate will firmly press your breast from above. This flattens your breast, holding it still while the x-ray is taken. The procedure is repeated for both breasts.
The three main types of mammograms include:
- Conventional mammogram: Takes 2D black and white film images of the breast.
- Digital mammogram: Like a conventional mammogram, it takes 2D black and white images of the breast. However, these images are entered directly into a computer, so the doctor can zoom, enhance, and better inspect the images.
- 3D mammogram: Takes multiple pictures during the test to develop a comprehensive 3D view of the breast tissue, shown to improve the diagnosis of cancer in dense breast tissues.
Some women say mammograms are uncomfortable, or even painful. However, the discomfort only lasts for a few minutes, and getting the right images are crucial to look for early signs of breast cancer or other problems.
If your mammogram is normal, continue to get mammograms so any changes over time can be easily compared. Even if the result is abnormal, it doesn't necessarily mean cancer. Your doctor may order additional scans or test, or refer you to a specialist, for diagnosis and treatment.
Does Medicare cover clinical breast exam?
Medicare Part B covers a clinical breast exam to check for breast cancer once every 24 months. This typically happens as part of the pelvic exam, also covered by Part B, and includes a Pap test to check for cervical and vaginal cancer.
If you're at high risk for cervical or vaginal cancer, or if you're of child-bearing age and had an abnormal Pap test in the past 36 months, these screenings are covered once every 12 months.
Why you should get a mammogram
Detecting breast cancer early makes it easier to treat, and it's more likely the treatment will be successful. Mammograms can help detect a lump up to three years before you or your doctor can feel it. The two most common types of breast cancer are:
- Invasive ductal carcinoma, when the cancer cells begin in the ducts and grow outside into other parts of the breast tissue, and even other parts of the body.
- Invasive lobular carcinoma, when cancer cells begin in the lobules and spread into the breast tissues that are close by, and can also spread to other parts of the body.
Identifying breast cancer early means you can get treatment faster, and it's more likely the treatment will be successful.
Breast cancer risk factors
The primary risk factors include being a woman and getting older, because most breast cancers are found in women who are ages 50 or older. Other risk factors include:
- Genetic mutations to certain genes, such as BRCA1 and BRCA2
- Early menstrual periods (before age 12) and starting menopause after age 55
- Having dense breasts, which can sometimes make it more difficult to see tumors on a mammogram
- Personal history of breast cancer or certain non-cancerous breast diseases
- Family history of breast or ovarian cancer
- Previous treatment using radiation therapy
Other risk factors include:
- Not getting enough physical activity
- Being overweight or obese after menopause
- Taking hormones, such as hormone replacement therapy or certain oral contraceptives
- Having the first pregnancy after age 30, not breastfeeding, and never having a full-term pregnancy
- Drinking alcohol
- Smoking
Just because you have risk factors doesn't mean you'll develop breast cancer, and some women can get breast cancer without any risk factors.
You can reduce your risk by keeping a healthy weight, exercising regularly, and limiting alcohol intake. If you take hormone replacement therapy or oral contraceptives, ask your doctor about additional risks. Additionally, if you have a family history of breast cancer or inherited changes in your BRCA1 and BRCA2 genes, your doctor may have additional suggestions for lowering your risk.
And finally, be sure to get your annual screening mammogram.
Symptoms of breast cancer
Some people don't have any signs or symptoms of breast cancer, but those who do may experience one or many of the following:
- A new lump in the breast or underarm
- Thickening or swelling of part of the breast
- Irritation or dimpling of breast skin
- Redness or flaky skin in the nipple area or breast
- Pullin in of the nipple or pain in the nipple area
- Nipple discharge (other than breast milk)
- Any change in the size or shape of the breast
- Pain in any area of the breast
Some of these symptoms can occur due to other conditions and don't necessarily mean cancer, but be sure to talk to your doctor right away to get the right treatment as soon as possible.
Additional resources
Understanding Breast Cancer
External Website Link
What Is Breast Cancer?
External Website Link
Mammograms
External Website Link
Breast Cancer Awareness: Do You Know the Signs?
Internal Website Link



