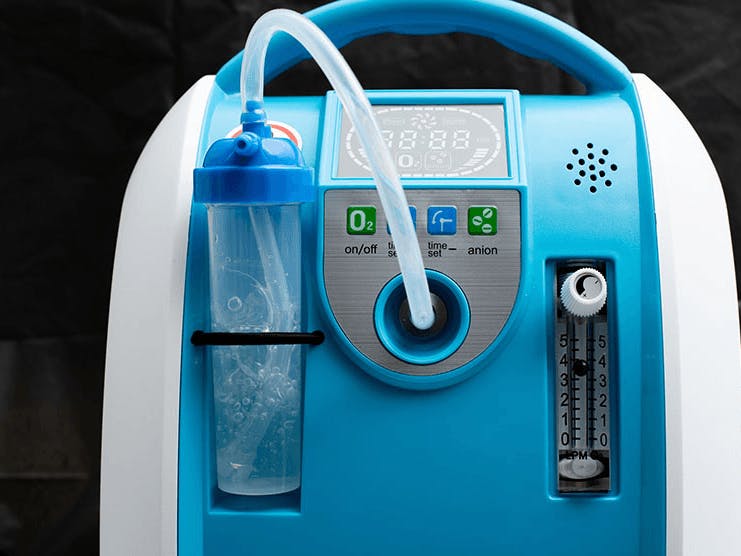
Medicare Part B provides coverage for durable medical equipment like portable oxygen concentrators - if you meet the qualifications.
Although it helps pay for a variety of oxygen equipment and accessories, Medicare only covers portable oxygen concentrators under specific circumstances.
The difference is in the word, "portable." Medicare coverage for durable medical equipment (DME) specifically states that beneficiaries must require said equipment for use in the home. For Medicare to cover portable oxygen concentrators (POC), your doctor must certify that you have a near-constant need for oxygen AND are mobile within your home. You must also meet all other requirements to qualify for an oxygen system.
Medicare coverage requirements for oxygen concentrators
All durable medical equipment coverage is through your Medicare Part B benefits. Therefore, the first requirement to qualify for DME is to be a Part B beneficiary.
Oxygen equipment eligibility depends on meeting each of the following criteria:
- Your doctor certifies that your body does not get enough oxygen
- Oxygen therapy may improve your health
- Your arterial blood gas values are within a certain range, which varies depending on the diagnostic method used and your particular condition
- Alternative measures to treat your condition have failed
In addition to the above criteria, you must use a Medicare-approved durable medical equipment supplier like Inogen. You can find a supplier on Medicare.gov here. Just enter your zip code and press Go. You can also call 1-800-MEDICARE for more information.
What does Medicare's oxygen equipment coverage include?
If you qualify for oxygen equipment, Medicare coverage includes a system to provide the oxygen, containers for oxygen storage, and oxygen-related accessories like tubing. If you need to use a humidifier with your oxygen machine, Medicare may also help pay for that.
Please note that, if you own your own equipment AND meet the qualifications listed above, Medicare Part B covers the oxygen contents and related supplies.
How much does oxygen equipment cost?
Medicare Part B covers oxygen equipment rental instead of an outright purchase. You must first meet the Part B deductible before Medicare begins paying its share. In 2023, the Medicare Part B deductible is $226.
Once you meet your annual deductible, you pay the standard Part B coinsurance of 20 percent of the Medicare-approved amount, with Medicare covering the remaining 80 percent.
The cost to rent oxygen equipment varies widely depending on the type of equipment, supplier, tank size, and more. On average, though, you can expect to pay around $140 per week for an oxygen concentrator rental if you don't have health insurance.
That price rises considerably when you add in the portability factor. Renting a portable oxygen concentrator costs around $210 per week on average.
Find a Medicare plan that covers portable oxygen containers
For either option, Medicare pays their 80 percent, leaving you owing between $30 and $40 per week, on average, for oxygen equipment rental.
These calculations assume that the Medicare-approved amount is about the same as the market price for oxygen equipment rental. However, Medicare typically contracts a much lower rate than the going market price. You'll need to call medical equipment suppliers in your area to get a better idea of what your cost would be.
What does oxygen equipment rental include?
Medicare oxygen equipment is rented for 36 months. In addition, medical equipment suppliers must furnish the oxygen equipment and related supplies for an additional 24 months if necessary.
Your monthly rental includes the following oxygen accessories and services:
- Tubing or mouthpiece
- Oxygen contents, including liquid oxygen and oxygen concentrate
- Maintenance (i.e. servicing and repairs as needed) of the oxygen machine
Medical suppliers must provide both the equipment and related supplies for up to 5 years, assuming you continue to have a medical need for oxygen.
What happens after 36 months?
If you still need oxygen after renting the equipment for 36 months, your medical supplier must continue maintaining the equipment and furnishing supplies for up to 5 years (this includes the initial 36-month period). The DME supplier must also continue supplying the monthly delivery of oxygen tanks or cylinders, for which you will continue paying the 20 percent coinsurance.
After 5 years, your current provider no longer has to supply oxygen equipment – even if you still have a medical need for oxygen. You can, of course, continue with this provider if you both agree. You may also choose a different durable medical equipment supplier and begin a new 36-month rental period.
When is home oxygen prescribed?
Your doctor may prescribe home oxygen if you have a medical condition that reduces blood oxygen levels. This is known as hypoxemia.
Symptoms of hypoxemia include:
- A pale or blueish tint to the lips and skin (known as cyanosis)
- Confusion
- Fast breathing or shortness of breath
- Increased heart rate
- Sweating with minimal exertion
A wide array of health conditions may cause hypoxemia, including:
- Asthma
- Chronic obstructive pulmonary disease (COPD)
- Cystic fibrosis
- Heart failure
- Lung disease
- Pneumonia
- Respiratory trauma
- Sleep apnea
Even though all of these issues may make it difficult for your body to get enough oxygen, a diagnosis of one of these conditions does not automatically qualify you for Medicare coverage. That requires diagnostic testing to determine blood oxygen levels. Only if those fall within ranges determined by the Centers for Medicare and Medicaid Services (CMS) will you be approved for oxygen.
How do doctors diagnose hypoxemia?
If your doctor suspects you have hypoxemia, they should order tests to check your oxygen saturation levels. This may include breathing exercises and blood gas testing. The least invasive testing method is attaching a pulse oximeter to your finger to check oxygen saturation. Blood gas testing, on the other hand, involves drawing blood.
If your oxygen levels drop to 88 to 93 percent, your healthcare provider will likely recommend medical oxygen therapy.
Final thoughts
Talk to your doctor if you recognize any of the hypoxemia symptoms listed above. Whether you have Original Medicare (Parts A and B) or a Medicare Advantage plan and require medical oxygen, your Medicare benefits will help cover the cost.
And to find the right Medicare plan for your unique needs and budget, try our Find a Plan tool. It's fast and easy to use - just enter your zip code to get started.
Additional sources
- ClearMatch Medicare: Find a Medicare Plan
- Centers for Medicare & Medicaid Services: Home Use of Oxygen
- Medicare.gov: Find Medical Equipment & Suppliers



