There is no annual out-of-pocket maximum when you have Original Medicare (Parts A and B), which could leave you owing significant medical debt. Medicare Supplement plans in South Carolina help pay some or even all of your healthcare expenses.
What is Medigap in South Carolina?
Commonly known as Medigap, Medicare Supplement Insurance helps pay your share of costs with Original Medicare. This includes Part A, which covers inpatient care, and Part B, which pays for outpatient services.
There are 10 standardized Medigap plans (A, B, C, D, F, G, K, L, M, and N). Not all insurance companies offer every plan and some Medigap insurers provide high-deductible versions of one or more plans.
"Standardized" means that each individual plan has the same benefits no matter where you live or which insurance company you choose.
Who qualifies for Medicare Supplement Insurance in South Carolina?
If you have Original Medicare and are age 65 or older, you qualify for Medicare Supplement Insurance in South Carolina.
The state does not require insurers to offer a Medigap plan to people who are under 65 and qualify for Medicare due to a disability. The South Carolina Health Insurance Pool (SCHIP) is available to high-risk Medicare beneficiaries. However, premiums are much higher than what over-65 Medigap beneficiaries pay.
What does Medigap cover?
South Carolina Medigap coverage varies according to the plan you choose. At a minimum, though, every Supplement plan covers your Medicare Part A coinsurance and gives you 365 more lifetime reserve days as a hospital inpatient.
The following chart demonstrates the benefits of each Medigap plan:
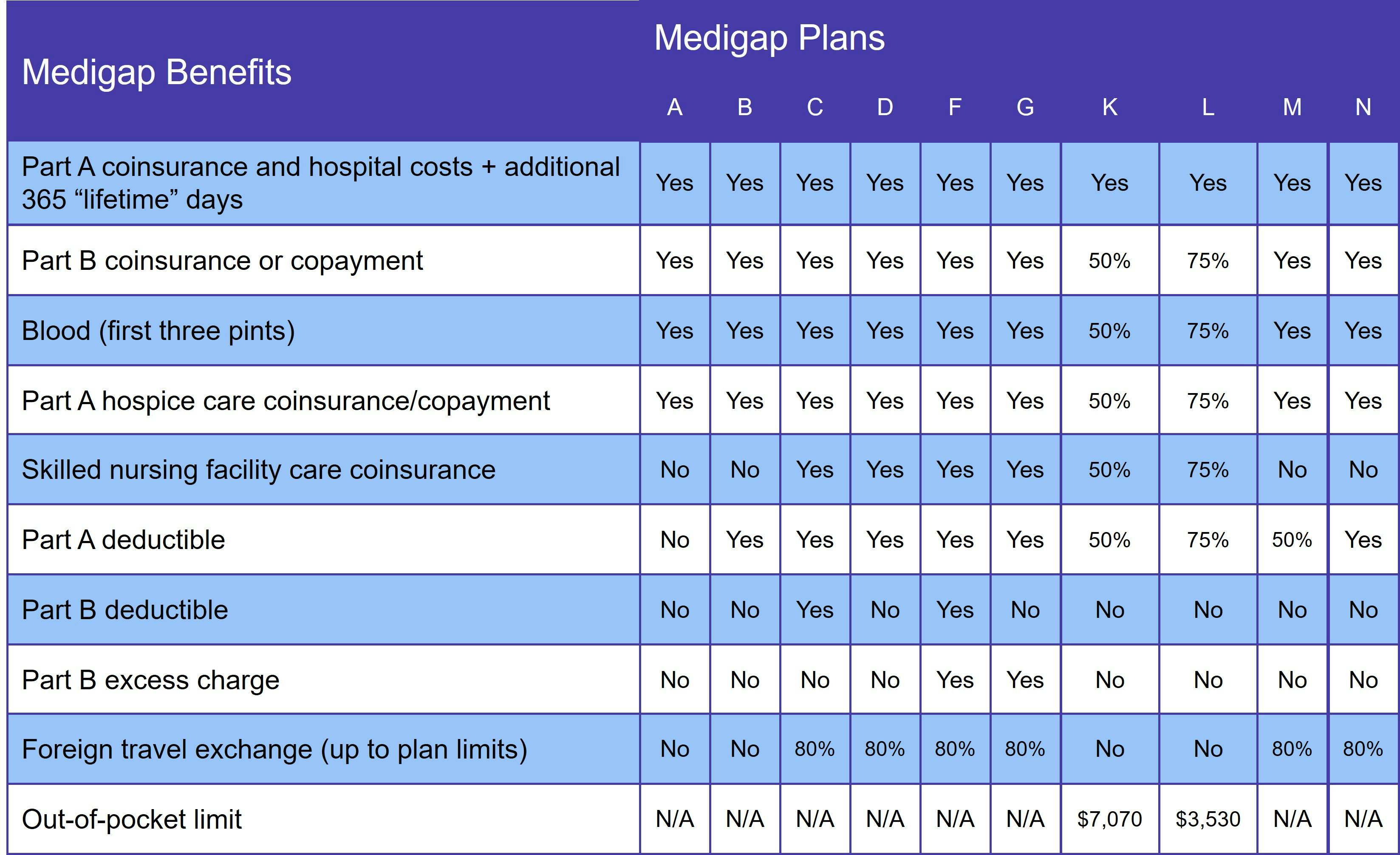
There are no longer any Medigap plans that provide prescription drug coverage. These benefits are available with a Medicare Part D prescription drug plan.
When is the best time to join a Medicare Supplement plan in South Carolina?
The best time to join a South Carolina Medicare Supplement plan is during your 6-month Medigap Open Enrollment Period (OEP). It begins the day you're both enrolled in Original Medicare and age 65 or older.
During your Medigap OEP, you have what Medicare calls guaranteed issue rights. You cannot be denied a Medigap policy or charged more for it, even if you have preexisting conditions.
You also get a Medigap OEP if you aren't yet 65 and qualify for Medicare due to a disability. However, state law only requires Medigap insurers to guarantee coverage; there is no limit to the premiums they can set for said coverage. Most under-65 beneficiaries pay much higher Medigap premiums.
These under-65 enrollees get a second OEP when they turn 65. At this time, your application is treated as if you'd never had Medicare.
Medigap Plan C and Medigap Plan F in South Carolina
A new federal law prohibits Supplement plans from covering the Medicare Part B deductible. Medigap Plan C and Medigap Plan F both provide this benefit, so neither plan is available to people who qualify for Medicare on or after January 1, 2020.
You get the same coverage (minus the Part B deductible) with either Medigap Plan D or Medigap Plan G.
How to choose a Medigap plan in South Carolina
To avoid the medical underwriting process, we recommend you choose the most comprehensive coverage you can afford during your Medigap OEP. You may not be able to find affordable Medigap coverage if you wait.
You should also look at pricing. Most Medigap insurers use one of three pricing methods:
- Attained-age rated: Premiums start out low and increase as you age. These plans cost the most over time.
- Community rated: Premiums are never based on age, making these plans the least costly option over time. Few insurance companies use community rated pricing.
- Issue-age rated: Premiums are based on your age when you join the plan but do not go up as you get older. However, they may rise due to inflation.
Our Find a Plan tool makes it easy to compare Medigap plans in South Carolina. Simply enter your location information to review Medicare plan options in your area.
